Among the types of cancer that your OB/GYN can screen for are uterine and endometrial cancer. Because uterine cancer is the most common type of gynecological cancer, it’s important to understand your risk as well as symptoms and screening options. Like all types of cancer, treatment for endometrial or uterine cancer is more effective when the disease is detected early, so it’s important to see your gynecologist regularly and follow their advice regarding screening or other tests.
What is Uterine or Endometrial Cancer?
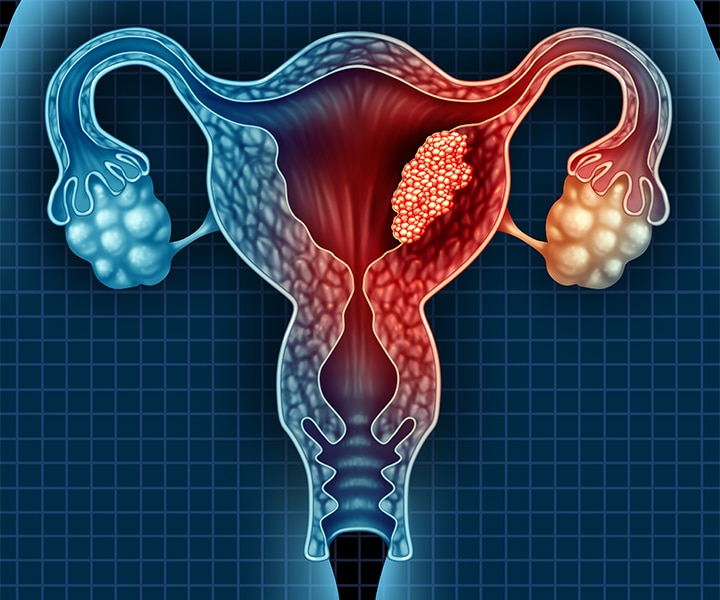
Uterine cancer is the most common gynecologic cancer in the United States. Over 90 percent of uterine cancers are endometrial, meaning that they start in the lining of the uterus (epithelium). The rest are mesenchymal, meaning that they originate in the uterine muscle wall and stroma.
What are Increased Risk Factors for Uterine Cancer?
Both environmental and genetic factors may increase your risk for developing uterine cancer. The most common risk factors in developing uterine cancer are:
- Obesity
- Diabetes
- Nulliparity
- Non-Hispanic Black women
- Unopposed estrogen
- Late menarche and late menopause
- Hereditary factors or genetic disorders, including Lynch syndrome
- Poly-cystic ovary syndrome (PCOS)
Of these common risk factors, those that present the highest risks for developing uterine cancer are obesity, lynch syndrome, and PCOS.
How to Prevent Uterine Cancer
There are some steps you can take which decrease your risk for uterine cancer. These include:
- Taking a combined birth control (estrogen and progesterone)
- Increasing parity (number of term pregnancies)
- Breastfeeding
- Eating a nutritious, balanced diet
- Maintaining a stable, healthy weight
What are Symptoms of Uterine or Endometrial Cancer?
The most common symptom of uterine or endometrial cancer is abnormal uterine bleeding outside of a menstrual period. For those who are 40 years old or older, endometrial cells on a Pap smear can indicate uterine or endometrial cancer. Finally, an imaging test such as a sonogram or CT scan for another purpose can incidentally find a thickened endometrial lining, which can indicate uterine or endometrial cancer.
How Do Doctors Screen for Uterine or Endometrial Cancer?
Your OB/GYN may screen for uterine or endometrial cancer in a variety of ways. First, they may perform a transvaginal ultrasound to determine an increased risk due to a thickened endometrial lining. A tissue sample screening through an in-office biopsy (dilation and curettage) with or without hysteroscopy may also be performed.
Schedule an Appointment
To learn more about screening or genetic testing options for uterine and endometrial cancer, schedule an appointment at Carnegie Women’s Health in New York, NY. Call our office at (315) 628-7063 or request an appointment online.
Frequently Asked Questions
What are the warning signs of uterine cancer?
Abnormal vaginal bleeding and/or discharge is the most common symptom of uterine cancer.
How are uterine and endometrial cancer treated?
Uterine and endometrial cancer may be treated in several ways depending on factors such as the patient's age, the stage of the disease, and side effects. For women with pre-cancerous cells in the lining of the uterus, hormonal treatment may be used, especially if that patient wishes to become pregnant and does not want a hysterectomy.u00a0 However, this requires close follow up and is not a safe option for some patients.u00a0 u00a0Hysterectomy, lymphadenectomy (removal of the lymph nodes in the pelvis and abdomen), and chemotherapy.
Who is more likely to get uterine cancer?
Women who are older than 50, who are obese, take estrogen by itself for hormone replacement, take tamoxifen, or have close family members who have had uterine, colon, or ovarian cancer may be at a higher risk of developing uterine cancer.
Will uterine cancer affect fertility?
Uterine cancer treatment may affect the ability to conceive, as the treatment usually involves removal of the uterus (hysterectomy). Some patients with pre cancer or very early, non invasive uterine cancer may be able to use hormonal therapy to treat the cancer and push off having a hysterectomy.u00a0 The risks of this need to be weighed carefully with the benefits. Patients with uterine cancer who wish to have children in the future are often encouraged to consider fertility options such as egg freezing and/or surrogacy.
Does obesity increase risk of uterine or endometrial cancer?
Excess adipose (fat) tissue can increase circulating estrogen levels, which will increase the risk of endometrial cancer.u00a0 Endometrial cancer is twice as common in overweight women and three times as common in obese women.