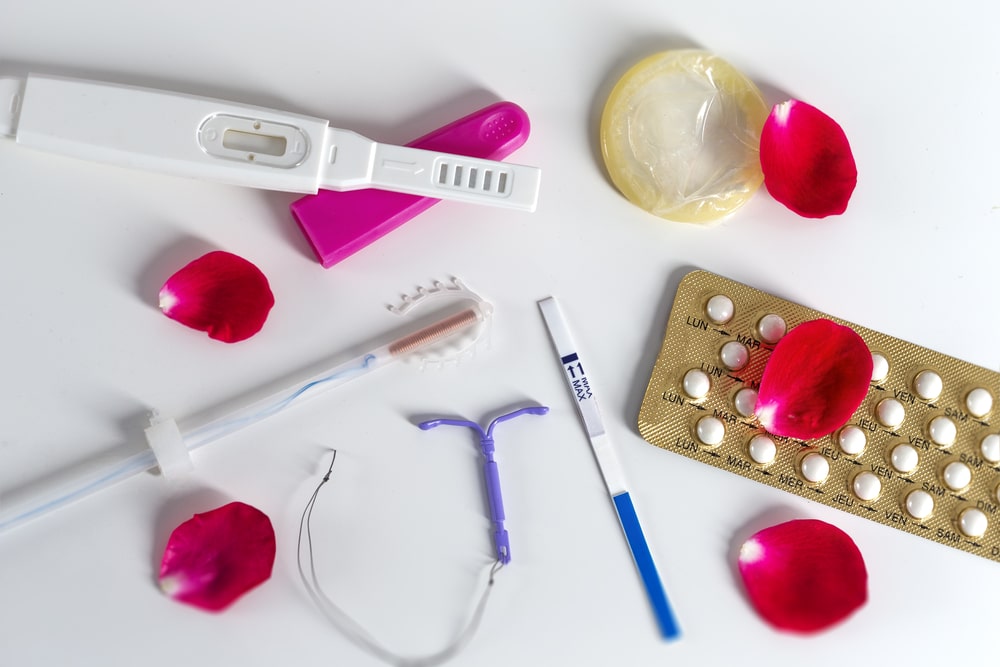
The vast majority of contraceptive methods have a potential for failure. The ones with the highest failure rate are the ones that require “user compliance”; two examples:
With condoms, using one every time you have sex and removing it in a timely manner.
With pills, taking one every day, not taking any competing medications.
Choosing which birth control method you are going to use to prevent a pregnancy or manage other health related symptoms is a very personal decision. There are multiple factors that can influence your choice of birth control, but it’s important to remember that there is no singular “best method”, just the one that makes the most sense for you and your needs at this point in your life. You may even decide that one type of birth control is not enough and that a combination of methods is what works best for you.
How to Choose a Birth Control Method
When choosing a birth control method, you should always seek advice and guidance from your OB/GYN. They can help you weigh your options and make informed recommendations based on your health and fertility goals. Asking friends and family about their experiences with different birth control methods can be helpful, but keep in mind that everybody responds differently to certain methods. Just because one worked like a dream for your sister, doesn’t necessarily mean it will be a perfect match for you as well, and vice versa. When you are choosing a method, here are some questions to consider:
For how long would you like to have effective contraception?
Is cost of contraception an important factor in your decision?
Do you need protection against sexually transmitted Diseases (STDs)?
Is there a plan for pregnancy in your future?
What Types of Birth Control are available?
There are several categories of birth control that are available.
Hormonal :
Hormonal methods can include pills, patches, vaginal rings, shots, subdermal inserts, or intrauterine devices.
Combination (estrogen & progesterone) pills, patches, and vaginal rings work by preventing ovulation (egg emerging from the ovary) as well as reducing menstrual flow; they require strict patient compliance with their use. When used properly are over 98% effective at preventing pregnancy, but when not used properly have a higher failure rate.
Progesterone only pills work by thickening the cervical mucus, limiting the ability of sperm to enter the uterus, and are about 95% effective at reducing pregnancy. They are often used during breastfeeding, which by itself (if you are nursing sufficiently to suppress your menses, therefore suppressing ovulation) is about 95% effective at reducing pregnancy. When these pills are used in breastfeeding women the overall effectiveness is over 98%.
Shots, subdermal inserts, and hormonal IUDs work by thinning the lining of the uterus, preventing implantation of a fertilized egg. These types of over 98% of the time, and don’t rely on user compliance.
Both hormonal types are also used to reduce menstrual flow
Intrauterine Devices (IUDs)
IUDs are small, T-shaped devices that are placed in the uterus by a doctor. There are two types of IUDs: hormonal and copper. A hormonal IUD (see above) prevents pregnancy by thickening the cervical mucus (preventing sperm from entering to uterus) as well as thinning the lining of the uterus preventing implantation should a sperm fertilize an egg.
Copper IUDs (no hormones) work by causing a “sterile inflammation” in the lining of the uterus, preventing the implantation of a fertilized egg. Copper IUDS often cause a heavier menses that could last 1-2 days longer than baseline.
The IUD Insertion procedure is typically done in the office in about ten minutes. Many patients do find it to be uncomfortable, especially those that have not had a vaginal delivery in the past. Timing your appointment to line up with your period, taking anti-inflammatories beforehand, and other techniques can often help make it more comfortable. Once in place, an ultrasound is performed two weeks later to ensure it has opened properly. IUDs are effective at preventing pregnancies for up to 10 years, depending on the type that you pick, making it a great low maintenance option.
Barrier:
Barrier birth control methods include condoms, diaphragms, cervical caps, and other devices that physically block sperm from reaching the egg. Because barrier methods, like female and male condoms, diminish or even block genital contact they also protect you from contracting or spreading most sexually transmitted infections.
Male Condoms: Pre-treated with spermicide to prevent any sperm seepage that could result in a pregnancy.
Diaphragm: Spermicide is applied by the user on the diaphragm before it is inserted into the vagina; the diaphragm remains in for six hours after intercourse.
Female Condom: Does not contain spermicide.
Behavioral:
Behavioral methods require the most patient motivation and compliance to enhance effectiveness. Comparatively speaking, these are the least effective in preventing pregnancy, with failure rates of up to 20-30%. These Methods include:
Calendar/Rhythm: By tracking the history of your menstrual cycle, you can predict when you will ovulate and abstain from having sex during the days of peak fertility.
Basal Body Temperature: By tracking the body’s temperature you may be able to predict when you will ovulate since there is a small increase in your temperature when you ovulate. Women who use this method will abstain from sex for three to four days after their temperature has risen and the week leading up to their suspected temperature drop.
Withdrawal (aka “pull out”): This relies on the male to “pull out” before ejaculating in their partner.
Overall, each form of behavioral birth control relies on the body and menstrual cycle being consistent and regular, which is not normally the case. In addition to being open to exercising extreme self-control, behavioral methods also have a steep learning curve.
Permanent Contraception:
If reversible birth control isn’t an option for you, there are several permanent contraceptive methods available. Sterilization can be performed on either partner:
Female Sterilization: This involves either tying or removing the fallopian tubes; this is done in a hospital or outpatient clinic under general anesthesia via laparoscopy (slender camera and surgical devices passed through your abdomen). Overall recovery is 1-2 weeks
Male Sterilization: Vasectomy or tying of the vas deferens (the tube that allows sperm to enter the ejaculate) is an in-office procedure with local anesthetic or an outpatient surgical procedure with IV sedation. The recovery is 1-2 days. After a vasectomy, there is an approximate 2-3 month delay until the sperm count falls sufficiently enough to rely upon this method alone.
When considering if surgical contraception is right for you, it is important to keep in mind that these procedures are not easily reversible and should be considered permanent. Be sure to talk to your OB/GYN if permanent sterilization is a method you or your partner have been considering.
Emergency Contraception (EC)
Emergency contraception (EC) refers to methods to prevent pregnancy after unplanned or unintended intercourse. There are several options for emergency contraception that you can use in the event your primary method of birth control fails. These are mostly available without a prescription. The success rate of emergency contraception is very closely connected to how soon after intercourse they are utilized. EC pills that are available at the pharmacy (often ‘behind the counter’, as opposed to being on the shelves) are most effective when taken within 3 days after unprotected sex. They have very few side effects, and when successful your period comes when it is expected.
If you have already been considering a copper IUD, it can also work as an effective emergency contraceptive for up to 5 days after unprotected sex but should only be inserted if you plan to use it long term.
Combining Birth Control Methods:
For maximal avoidance of pregnancy as well as sexually transmitted diseases, many couples employ more than one contraceptive method simultaneously. An example of this would be a woman who uses condoms for contraception and STD prevention and also takes oral contraceptives in case a condom fails. Another example would be a patient taking progesterone only oral contraceptives and using vaginal suppositories with intercourse. Alternatively, you may choose to pair behavioral methods, such as basal body temperature or calendar with withdrawal.
It’s important to remember that only condoms protect you against STDs. Making sure to add a barrier method, like male or female condoms, onto your chosen hormonal or permanent contraceptive method is a great way to reduce your risk of contracting STDs.
Finally, ask your doctor before combining two methods that involve a medical device or hormones, such as an IUD paired with emergency contraception. Often, pairing two hormonal options won’t increase the effectiveness of either, and may result in unwanted side effects. Ultimately, you should always discuss your birth control plan with your OB/GYN to make sure your method for preventing pregnancy is best suited to meet your health and fertility goals.
Schedule an Appointment
To schedule an appointment with Carnegie Women’s Health, call our New York office at (315) 628-7063 or request an appointment online.